Breastfeeding and Low Supply: Common and Surprising Causes and Solutions
 Monday, August 19, 2013
Monday, August 19, 2013 Low milk supply is always listed as a top reason why mothers quit breastfeeding and switch to formula. Experts often claim that the percentage of women who can't produce enough milk is extremely small (usually numbers under 5% are quoted, without any specific source being given). However, the number of women who say they tried everything and still couldn't make enough milk seems to be on the rise. This article explores some of the possible reasons for that, including polycystic ovary syndrome (PCOS), diabetes and pre-diabetes, and mammary hypoplasia (insufficient glandular tissue).
 Image credit: Daquella manera on flickr
Image credit: Daquella manera on flickr
Why do so many mothers struggle to make enough milk?
In Bangladesh, where infant formula isn't readily accessible, affordable or safe for most families, 98 percent of babies are breastfed and the average age of weaning is 33 months (source: WHO Global Data Bank on Infant and Young Child Feeding). In Norway, a country well known for having created perfect conditions for breastfeeding, around 80 percent of babies are still being breastfed at six months of age (source: Suzanne Barston, Bottled Up). Norway's 80 percent is significantly higher than in countries like Canada, the United States, and the United Kingdom, but it is also a far way off from the 98 percent in Bangladesh.
So what is the difference? I think part of it is certainly choice. Although formula feeding may be frowned upon in Norway, ultimately, women still have the option not to breastfeed. Infant formula is accessible and Norwegians generally have the financial means to be able to afford it. Some women may simply not want to breastfeed or may find it too difficult and they have the freedom to make that choice. A mother in Bangladesh, however, would have to grit her teeth and push through.
Beyond the issue of choice, another element that is worth considering is that there are certain medical conditions that are more prominent in Western developed countries that can have an impact on a woman's ability to produce enough milk. In particular, many medical conditions that create fertility challenges for women can also cause low milk supply. While there have been advancements in fertility treatments in the Western world, allowing women with fertility challenges to have babies, those same women may not be aware that they could have trouble breastfeeding as well.
In developing countries, some of the conditions that can cause infertility are less common than in the developed world. Additionally, women facing infertility in developing countries are probably much less likely to end up having a baby because they don't have access to the same types of medical treatment we do in the Western world. So our advancements in the area of fertility treatments may unintentionally be increasing the percentage of mothers who will struggle to produce enough breastmilk. Unfortunately, health care providers and other sources of breastfeeding information are not preparing mothers who struggle with infertility for the fact that they may struggle to breastfeed their baby.
Common Causes of Low Supply
Before we get into the medical conditions that can cause low supply, it is important to note that there are a number of fairly common and well known causes of low milk supply that primarily have to do with breastfeeding management. These factors are generally easily to control and don't require much more than a good understanding of breastfeeding best practices and the law of supply and demand.
At a very basic level, when milk is removed from your breast, that sends a signal to your body to make more. The more milk that is removed, the more milk your body makes. The less milk that is removed, the less milk your body makes.
- Scheduling or timing feeding: If you're getting advice from an older generation or from misguided baby training books, you may think that you should be trying to get your baby on a schedule or that you should be feeding for a specific amount of time at each feeding. This is not the case at all. Scheduled or timed feeds can make your baby go hungry and tamper with your milk supply. The best way to establish and maintain a strong milk supply is to breastfeed your baby on demand. You can't nurse too frequently, but you can nurse too infrequently. Newborns should be nursing 10 to 12 times per day. If you're not sure what signs to watch for, check out the information on Hunger Cues on kellymom.com. It can sometimes be hard to read those cues during the early days, so when in doubt, put the baby to your breast.
- Skipping a feeding or supplementing: Breastfeeding can be overwhelming and all consuming. Sometimes moms just want to get a bit more sleep or want to go out for a bit without the baby. So they leave their partner or someone else in charge of giving a bottle. Unfortunately, if the mom doesn't then pump during the time when that bottle is being given, it will send signals to her body to make less milk and that can decrease her supply. If giving a bottle (without pumping to replace it) becomes a regular habit (e.g. once per day, several times per week), it can significantly impact the mom's ability to produce enough milk. The early days of breastfeeding are especially critical for establishing a strong milk supply and nursing frequently and not skipping feedings is very important. In particular, mothers whose babies who receive a non-breastmilk supplement in hospital during those first few days after birth are much more likely to not meet their own breastfeeding goals.
There are numerous other possible causes of low supply including some medications, hormonal birth control, retained placenta, poor latch, nipple confusion and more. For more information on getting established with breastfeeding, check out the article Breastfeeding Your Newborn on kellymom.com.
Lesser Known Causes of Low Supply
What if you're doing everything right and your body still isn't making enough milk? In addition to the common reasons for low supply, there are a number of lesser known causes of low supply that often catch new mothers by surprise. Many of these seem to be more prevalent in the developed world than in the developing world, which may be one reason why such a large proportion of mothers seems to struggle with low supply in the Western world. All of the causes described below have the potential to impact a mother's milk supply, but it doesn't do so consistently. Some mothers with these medical conditions will struggle with breastfeeding and others will have no problem at all. But all women with these conditions apply should be aware that it could impact their ability to breastfeed their baby.
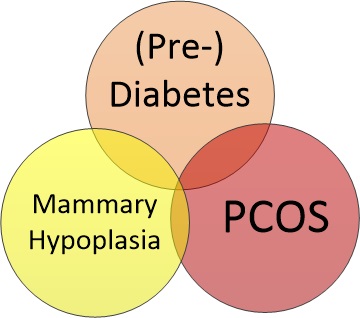 The first three conditions that can impact milk supply are, in many cases, related. Women who have one of these are often prone to the others as well.
The first three conditions that can impact milk supply are, in many cases, related. Women who have one of these are often prone to the others as well.
Diabetes and Pre-Diabetes
Scientists have discovered a link between insulin and breast milk production. Mothers who have low levels of insulin may also have trouble producing enough milk. This will be of interest and concern to mothers with diabetes, of course. However, it may be an even bigger problem for mothers who have pre-diabetes or undiagnosed diabetes. If they do not have a formal diagnosis and are not doing anything to control their insulin levels, this could unknowingly make it difficult for them to produce enough milk. Diabetes rates have doubled in the past 12 years, in particular among young women. As diabetes rates increase (and especially as the number of undiagnosed cases of pre-diabetes and diabetes increases), the number of women who have trouble breastfeeding their babies is likely to increase too.
Polycystic Ovary Syndrome (PCOS)
Polycystic Ovary Syndrome (PCOS) is one of the most common female endocrine disorders and can affect a woman's hormone levels, periods, ovulation, fertility and ability to produce enough milk when breastfeeding. According to research by Dr. Charles Glueck, MD Medical Director of the Cholesterol and Metabolism Center at he The Jewish Hospital - Mercy Health, PCOS affects around six to eight percent of Caucasians, eight to 10 percent of African-Americans and 10 to 12 percent of Latinos and Native Americans. Lisa Marasco, MA, IBCLC, notes that PCOS is related to a number of possible reasons for lactation problems, including hyperandrogenism (can inhibit mammary development and milk synthesis), insulin resistence, hypothyroidism, and possibly too much estrogen. She notes that "PCOS is a collection of different pathologies. A woman with one or more of these problems may or may not have a diagnosis of PCOS, but can still be affected." According to Dr. Anita Swamy, Medical Director at he Chicago Children's Diabetes CEnter at La Rabida, there is a strong link between PCOS and diabetes: "While type 2 diabetes risk factors such as insulin resistance and glucose intolerance are often seen in patients with PCOS, PCOS itself confers a significant risk, up to 10-fold versus the normal population, for development of type 2 diabetes."
Mammary Hypoplasia / Insufficient Glandular Tissue (IGT)
Some women do not have enough glandular tissue to nourish a child. According to noteveryonecanbreastfeed.com, "women with Insufficient Glandular Tissue may have experienced a lack of breast changes during puberty and/or pregnancy, no engorgement, and a low milk supply." According to The Breatsfeeding Answer Book (referenced on LLLI), 1 out of 1000 mothers experiences primary lactation failure. This can be due to hypoplasia or other causes. However, like with diabetes and PCOS, assisted fertility and hormonal support to conceive babies is leading to an increase in the number of cases of babies born to mothers with hypoplasia. Not a lot is known about the causes of mammary hypoplasia, but there is likely a genetic link (women who have it often say that no one in their family was able to breastfeed). For more information see Supporting Mothers with Mammary Hypoplasia by Diana Cassar-Uhl, IBCLC on LLLI, her article on hypoplasia/IGT on kellymom.com and the website NotEveryoneCanBreastfeed.com.
Breast or Nipple Surgery
Another possible cause of low supply is breast or nipple surgery, which can include breast augmentation, breast reduction and other types of breast or nipple surgery. According to BFAR.org (a website dedicated to providing information and support for breastfeeding after breast and nipple surgeries), there are many factors that affect how much milk a mother can make after surgery: "The condition of her ducts is very important, however, that the state of the nerves that affect milk release is equally critical. Fortunately, the ducts and nerves can regenerate through processes known respectively as recanalization and reinnervation, which are critical to the impact of breast surgery upon milk production and release." Mothers who have had breast or nipple surgery are often able to breastfeed, but may not be able to establish a full supply. This doesn't mean that it isn't worthwhile and, as the book on breastfeeding after reduction surgery by Diana West, IBCLC is titled, you should Define Your Own Success.
Solutions for Low Supply
If you have a newborn and are worried that your baby isn't getting enough milk, first check kellymom.com's page on Low Supply, in particular the section called Is your milk supply really low?.
If you are a mom with one of the conditions discussed above, there are some things that you can do to help prepare for breastfeeding. I know people with these conditions who struggled significantly with breastfeeding their first child, but were able to successfully breastfeed their second child because they were more informed and more prepared.
- Gather Your A-Team: If you want to breastfeed, having the right people around you in the right environment is critical. This requires doing the same things every mother should do to get breastfeeding-friendly prenatal care, hospital and pediatrician, but it may also mean seeking out certain specialists who have experience working with mothers with your condition and knowing how you can access them for support and expertise before and after your baby arrives.
- Learn More About Your Condition: Women should do research into their own individual situation to find out what their chances of being able to breastfeed are and to learn about possible solutions. Consult your healthcare provider and experts in the field who are knowledgeable about lactation. For example, as it relates to PCOS, Lisa Marasco, MA, IBCLC suggests: "Be aware of your individual PCOS issues. Insulin resistence? Androgen problems? Do everything in your power to address these, before conception preferably but even during pregnancy. Have someone assess overall breast development, especially if the mother herself has any concerns. Seek a consultation with a lactation consultant if breasts are unusual or are not growing/changing during the pregnancy."
Once your baby arrives, you will want to get breastfeeding started as quickly and as well as possible. This includes doing the same things any mother would do for good breastfeeding management (nursing frequently, on demand, etc.), but may involve doing a bit more.
- Remove as much milk as possible in the first two weeks: BFAR.org suggests removing as much milk as possible from your breasts in the first couple of weeks. This is because the supply of breast milk is determined by demand, so the more you remove the more you make. This certainly involves breastfeeding as frequently as possible, but could also involve some pumping with a high quality, hospital grade, double electric pump. Being able to pump hands-free will make it easier for you to get through those times and not feel chained to the pump (you can read, eat, use the computer, tickle the baby, etc. while pumping hands-free). Lisa Marasco, MA, IBCLC suggests offering the breast right from the start and keeping the baby skin to skin during early days to encourage more nursing.
- Address any concerns immediately: If you have latch problems, plugged ducts, or other breastfeeding problems, address them right away. The longer you wait, the more likely these regular nursing problems are to have an impact on your supply that may not be easy to recover. If the baby is sleepy or not latching well, pump after feedings to ensure you're removing more milk from the breast.
- Identify and address your risk factors: When working with mothers with PCOS, Lisa Marasco, MA, IBCLC tries to identify and address their risk factors. For example: "Metformin, for instance, reduces insulin resistance. This in turn can help reduce androgens. Normalizing the hormonal milieu during and after pregnancy is going to give mom the best chance. I also may suggest specific herbal galactogogues—for instance, goat’s rue is reputed to stimulate mammary development and milk production. It has anti-diabetic properties and is the herb that metformin was developed from, making it especially appropriate, I think, for PCOS. Fenugreek has similar properties, and I also like saw palmetto and fennel for both mammary stimulation and anti-androgen action on top of stimulating milk production."
- Medications that increase milk supply: Depending on where you are located, there may be certain medications you can access to increase your milk supply. For example, in Canada many doctors will prescribe Domperidone according to the recommendations of renowned breastfeeding expert Dr. Jack Newman. Domperidone isn't easy to access everywhere though, so speak to your lactation consultant and physician to find out what options are available to you.
- Supplementing at the breast: No matter how much milk you make, there are benefits to you and your baby for feeding at the breast using a system such as Lactaid. Feeding at the breast boosts the baby's immune system through skin-to-skin contact, better develops the jaw muscles, and fosters that wonderful bonding experience that every new mother and baby pair need and crave. You can use your own pumped milk, donor milk, infant formula, or some combination thereof. For more information see Yes, You CAN Breastfeed Successfully No Matter How Much Milk You Make on Best for Babes. If you are supplementing via bottle, see their guide on bottle feeding.
In addition, if you are a healthcare provider working with a woman with diabetes, PCOS, hypoplasia or other conditions that impact her fertility, it is important to talk to her about the potential impact on her ability to breastfeed. Surgeons performing breast and nipple surgery should also make lactation a topic of discussion for women who are considering surgery. The more information a woman has before she gets pregnant and before the baby arrives, the better prepared she will be to make decisions about breastfeeding and to prepare herself for breastfeeding.
Other Resources
If you're looking for more information on low milk supply, the following articles and books provide excellent information.
Hidden Hindrances to a Healthy Milk Supply by Becky Flora, BSed, IBCLC
Increasing Low Milk Supply by Kelly Bonyata, BS, IBCLC
How does milk production work? by Kelly Bonyata, BS, IBCLC
Buy The Breastfeeding Mother's Guide to Making More Milk by Diana West, IBCLC and Lisa Marasco, MA, IBCLC on Amazon.com or Amazon.ca (affiliate links)
Your Story
Did you have difficulty breastfeeding as a result of low supply? If you have diabetes, PCOS, breast reduction surgery or other conditions mentioned in this post, did your health care providers talk to you about the possible impact on your ability to breastfeed? If you breastfeed or attempted to breastfeed more than one child, was it easier the second time around?
 Breastfeeding,
Breastfeeding,  Mom's Health and tagged with
Mom's Health and tagged with  PCOS,
PCOS,  breastfeeding,
breastfeeding,  diabetes,
diabetes,  insufficient glandular tissue,
insufficient glandular tissue,  low supply,
low supply,  mammary hypoplasia,
mammary hypoplasia,  polycystic ovary syndrome,
polycystic ovary syndrome,  pre-diabetes
pre-diabetes 



















Reader Comments (42)
I think if I'd been told that PCOS would give me low milk supply before my child was born I might never have started breastfeeding but I wasn't. My mum (who also had mild PCOS) told me she suffered from oversupply while nursing and my sister (another one with PCOS) definitely had over supply, I too was able to provide more than enough for my baby's needs. It is my understanding that nearly one third of women with PCOS will suffer with over supply. (http://kellymom.com/bf/concerns/mother/pcos/)
PCOS is only one small aspect of infertility however and for nearly a third of heterosexual couples receiving ART (Assisted Reproductive Technology) their infertility is undiagnosed. Feeling let down by our own body's ability to reproduce, sub-fertile women can be easily convinced that their body will let them down again when it comes to breastfeeding. Yes sub-fertile women need information but more than that we need the support and encouragement to help us succeed.
As someone who helps and supports women with PCOS, hypoplastic breasts and women who have had breast surgeries to successfully breastfeed, I'm surprised your article doesn't mention midwives in your list of care providers who can be of help. Midwives in Ontario have very high rates of breastfeeding initiation and rates at 6 months. Thanks for considering this addition.
Thanks Annie, for a great post full of resources. You highlight that low supply can be complicated but with the right support many women can meet their breastfeeding goals. I just wanted to add that food allergies and poor intestinal health (which often lead to nutritional deficiencies) can also play a significant role in the ability to produce milk.
THANK YOU for such a great article.
I struggled with low supply with my son three years ago. With Domperidone, herbs, pumping 5-6x a day on top of breastfeeding, I managed to work up to about 80% of what he needed & supplemented from 12 days to 10 months. I'm still not sure exactly what it was that caused my issues, as there were so many problems with management in the early days, plus I suspect I may have IGT to some extent.
I'm pregnant again, due in early September & I've got a plan lined up & my support people all in place. I'm cautiously optimistic that I can avoid having to supplement & pump constantly this time around, but who knows?
Even if I do have issues again, I'd be happy if it turned out similarly, as I breastfed my son until he nearly self-weaned at 29 months. I'll be proud if I can say I have breastfed two children past two years each. :)
This is an excellent article, and I'm linking to it on my prenatal/postpartum support FB page. Thank you for writing it! I'm currently taking a lactation support class (taught by RN and IBCLC Gini Baker, who trains many doctors, nurses, doulas, teachers and other breastfeeding counselors/educators), and it has really opened my eyes to many of the points you make -- including the possible relationship between fertility issues and breastfeeding issues (and between breast augmentation and breastfeeding issues).
It's also a good idea to remind everyone that your supply is low BY DESIGN when your baby is born. Colostrum is present in very small amounts because your baby is not born hungry. Your baby is born full of meconium (poop) and has a high suck need, but does not actually need to *eat* a lot (she DOES actually need to *nurse* a lot). Your milk volume should increase around day 4, but a low volume in the early days does not mean you have to be worried you have a low supply.
I would add that, within those crucial first few weeks, days 0-3 (and the first two hours) of your baby's life are incredibly important to setting you up for a good milk supply. The first three days are when your baby's sucking reflex (and high suck need) are helping build the prolactin receptors that will tell your body to build more milk. The first 2-3 hours are the "golden hours" for mom and baby bonding (first latch takes an average of 56 uninterrupted skin-to-skin minutes). We need to get the word out about breastfeeding in the earliest days (when many moms are undersupported and may still be in a hospital). And skin-to-skin and baby-wearing time can be such a boon during these days.
[This is, of course, NOT to say that mothers and babies who are separated during early hours or days (hopefully due to medical necessity, and not routine hospital policies) will be unable to build a great breastfeeding relationship. It may be another issue to work through, though.]
I also think we need to be reminding moms prenatally and in early postpartum that there is a growth spurt (and therefore, a temporary increase in nursing) coming around 2 weeks, so that they don't get discouraged and think they have low supply when their baby seemingly "wants to nurse around the clock."
Speaking of the hospital and spreading the word, it's also so important that women who may choose an epidural during labor know that they may end up with "third spacing," swelling due to a high level of retained fluids from their IVs (routinely given during epidurals to keep BP low), and that this edema (swelling) can occur in the breasts, making the nipple very hard for baby to latch on to. So everyone needs to know a technique called Reverse Pressure Softening, which helps move that fluid out of the way so baby can continue to latch on 8-10 hours after birth (when the swelling occurs).
http://kellymom.com/bf/concerns/mother/rev_pressure_soft_cotterman/
Excellent article, thanks!
Just one nitpicky thing - women (or anyone) with prediabetes or Type 2 DM would have a higher insulin level (not low like you listed), but they would have insulin resistance such that their body can't properly/easily metabolize insulin. So as a result, more insulin is produced. It's only in Type 1 DM that there would be low/no insulin production, but Type 2/prediabetes would be much more relevant in this situation (as it's the Type 2 DM rates that have increased in young women, as you've mentioned/linked).
Jen: Thank you for the comment. The recent research on breast milk production and insulin that I linked to in the post above has actually been focusing on mothers with Type 2 diabetes. I'm typing on an iPad now, so I won't repeat all the details, but you can read them in that link.
RM: My intention wasn't to exclude any type of health care provider, which is why I said "health care providers" generally rather than listing them all. That would certainly include midwives.
Liz: Yes, encouragement is critical for all moms. I focused on information in this post because of the number of women I've met with PCOS who were incredibly let down when they couldn't make enough milk. I think being prepared ahead of time would allow them to mentally prepare for the possibility, but also take steps to have the bet shot possible.
My first child was severely tongue tied and I wasn't prepared at all. It was a nightmare, ending with him latching on for the first time at 7.5 weeks old. With my second child, I had a plan in place and was prepared. She wasn't tongue tied, but if she had been, I was ready to have it diagnosed and dealt with immediately.
I think actually the "Daily Mail" (your link) has it wrong when they list "mothers who are struggling with feeding may have low levels of insulin" (missed that phrase before in the article) - because the correct mechanism for Type 2 diabetes/prediabetes is as they mention later in the article, "it takes longer for milk to come in to women whose bodies struggle to metabolise enough insulin" - those with Type 2 DM/prediabetes can't metabolize enough insulin and thus they have higher levels of insulin overall (not lower levels). I will try to check the original research later to check if it was an error of the newspaper/website (and make sure the researchers haven't come across something totally opposite to the known mechanisms ;-) ).
Only reason I point it out, is that if women with PCOS or at risk for diabetes (eg family Hx, obesity) who are pregnant and wondering if there might be issues with breastfeeding want to check what their insulin level is like, I'm pretty sure it would be a high serum (fasting) insulin that they should be concerned about (ie. insulin resistance - the confusion arises because yes, there is a lower level of insulin being used/metabolized, but the blood test would show a high level).
Ok, found the actual press release that the Daily Mail article was most likely taken from. It refers to "sub-optimal glucose metabolism", "low milk supply due to insulin dysregulation", "mammary gland becomes highly sensitive to insulin during lactation", but never refers to low insulin levels. So, I think the Daily Mail journalist was inaccurate in her writing - and if any women are concerned and ask their doctor for a fasting insulin test, it should be a high insulin level they'd worry about.
http://www.eurekalert.org/pub_releases/2013-07/cchm-nsr070113.php (because my html never works right ;-) )
I have PCOS and was never told it could affect my milk supply! I really wish I had been told! My son is now 3 months old and despite the fact that I struggle with making enough milk for him I still go at it strong. BUT if I had been told then I would have done alot more before now (now that I DO know) to help make sure my crazy hormones didn't make it hard on me to feed my baby my milk! I want to thank the author for this article because now that I know this I will be doing whatever I can to see if it helps my milk supply!
@Jen, actually a person with Type 2 diabetes can indeed have lower levels of insulin depending on where they are on the disease spectrum.
@Kate - yes, well along in the course of Type 2 DM the amount of insulin can drop - but in the context of "However, it may be an even bigger problem for mothers who have pre-diabetes or undiagnosed diabetes" as written above, they would have higher levels /insulin resistance not low levels. Sorry if I wasn't clearer with that. I know that as a family physician, I just didn't want women thinking that "if I ask to get my insulin level tested, I should worry about future milk production if I have a low level" when it would be a high level that would indicate insulin resistance and possible pre-diabetes (and in the original article, also potential lower milk production).
It's always great to see an article that looks to help find reasons and solutions for difficulties breastfeeding (rather than just telling people they should!). Thank you for that. I did want to point out that Bangladesh has an infant mortality rate more than 10x that of Norway (49/1000 vs. 3.5/1000). Infant mortality is a complex issue related to health and safe resources but not all breastfeeding problems are solvable and alternatives have saved lives.
@Rebecca:
Yes, the infant mortality rate in Bangladesh is higher than in Norway. The rate is 37 deaths per 1000 live births, down from 130 in 1980 (source: http://data.worldbank.org/indicator/SP.DYN.IMRT.IN). That is significant progress and the downward trend is continuing through excellent public health initiatives and development work in the country (including improving breastfeeding practices). The causes of infant mortality in Bangladesh have been studied and include: Birth asphyxia (45%), prematurity/low birthweight (15%), sepsis/meningitis (12%), respiratory distress syndrome (7%), and pneumonia (6%) were the major direct causes of death (http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2965329/). Greater availability of infant formula wouldn't impact most of those causes. The only place I can see it contributing would be if there was a combination of prematurity/low birthweight with a mother's inability to produce enough milk. Addressing the issues that lead to premature births and low birthweight (e.g. maternal nutrition, prenatal care, etc.) would be more successful in addressing that issue.
I do think it is a good thing that mothers have choice in how they feed their babies in the developed world, but I think we need to be careful in equating a lack of infant formula to deaths in developed countries.Making formula less accessible in the developing world has saved lives by ensuring babies aren't fed formula made with contaminated water, that formula isn't being watered down, and that mothers do not lose their milk supply when they begin supplementing with formula.
Thyroid conditions can also affect milk supply. I've been researching iodine supplementation lately and I am truly curious if a deficiency could cause milk production problems. I have found no research on the topic, but have some accumulated some circumstantial evidence. 1) The recommended daily allowance for iodine is based on the thyroid's needs, but does not take into account the iodine your breasts collect for "proper breast function" 2) The hormones your thyroid regulates influence lactation. 3) Your thyroid needs iodine and selenium to function correctly. I no longer have any nurslings, and did not have a production problem either, but I am very curious to see if supplementation would help anyone.
Very useful article with valuable information! All pregnant women and new mothers should read this.
I wanted to respond with my own story of low supply with my first daughter and how it changed with my second. Both daughters had latch issues in the beginning, and under the care of an IBCLC I was given a nipple shield to help. My first daughter used it for 3+ months, my second for a few weeks. Initially my supply was very high with my first daughter. I had good milk transfer with the shield, and she gained well if on the slow side. Somewhere around 4 months her weight started to slow noticeably, and at 6 months we knew there was a significant problem. Her pediatrician asked a few questions and informed me that I must be making enough milk but it wasn't "good quality" and that I needed to supplement with formula post haste. I didn't, but instead went back to the lactation department at the hospital and realized I was producing far less, despite her nursing 10-12 times per day. After much work at the pump, renting a high end scale for pre/post feeding weight checks, and finally some domperidone ordered online I was back to producing. I asked my GP for a blood test to check my prolactin levels and they were low even for a non lactating woman. With no known endocrine disorders, nor diabetes/pre-diabetes, I still do not fully understand what could've happened.
Five years later and I am nursing my second daughter with no supply issues what so ever. Both births were c-sections (1 placenta previa, 2 footling breech), both daughters nursed exclusively and on demand to 6 months, neither with any oral issues... I don't think I'll ever know exactly what happened, but if I'd listened to my first daughters pediatrician I wouldn't have been successful in breastfeeding my eldest to 30 months, and may have been discouraged with my second (who is 8 months and still nursing strong).
I second that low levels if thyroid hormones are linked to low breast milk production. Thyroid dysfunction is also linked to diabetes. It's something that is not often tested for but really should be. Thanks for the great article.
My little one was born 5 weeks early and super tiny. His cheek muscles were underdeveloped and not strong enough to latch properly. The NICU nurses said a shield would make things easier for him. Being a first time mum I nodded along. The shield worked but there was never any discussion about how to eventually get him off the shield. I swore I'd never do it again but my little guy tired quickly and could rarely get enough through the breast. He was tube fed with a combination of breastfeeding for the first three weeks of his life in the NICU. I pumped and pumped and pumped so that he could at least get breast milk through the tube feedings. I was so worried about my milk supply. I was afraid it would get confused between pumping and feedings. When we finally got home I continued to breast feed until he developed colic and would have total meltdowns when trying to latch. I had to break down and pump and feed it to him through a bottle because it was the only way to get the breast milk into him. Anyway, the NICU and breastfeeding are sometimes not conducive to a high supply of milk, at least in my case. Sometimes with premies it's hard to set up those good habits early on because they're just not strong enough. It's shitty.
As some who has had low supply:
I wish that all women knew that breast feeding failure and low milk supply are not because the mother is "just not trying hard enough". No one should get to judge who is trying hard enough in this arena.
I wish that pregnant women knew what a lactation consultant does and when to consult one. Despite attending La Leche League meetings while pregnant and reading books about breastfeeding I didn't know that lactation consultants did weighed feeds or that if my child was diagnosed with failure to thrive it was time to see one.
I wish there was consumer awareness among mothers that not all who advertise themselves as lactation consultants are International IBLC certified. Also not all who advertise as IBLC certified actually are. There is a difference between lactation trainers, lactation counselors and lactation consultants that are IBLC certified. If someone is facing serious nursing problems they need the last one.
I wish there was a treatment protocol that took into account the well -being of mothers and babies. Asking a new mother who is looking after a newborn to pump every two hours around the clock may not be in the best interest of a mother recuperating from childbirth.
Lastly, I wish there was more awareness in the community about the 2012 Health Canada statement about the risks of using Domperidone. See following link http://www.breastfeedinginc.ca/AdvHTML_Upload/pdfs/Domperidone_Consensus_Statement_May_11_2012.pdf
Thanks for your post on this topic and for bringing awareness to this issue.
I thought I had low milk supply and tried every possible herb to increase it, but turns out I was making plenty of milk -- I just had an "exit problem" due to severely inverted nipples. I wasn't diagnosed until my second baby.
*Warning: I have to vent/rant* Well, I just read this. And it's a little too late for me. I wish I knew then what I know now... I agree that support is the most important thing to help resolve any issues that may be pre-existing or come up. I, unfortunately, was unable to breastfeed as I had hoped and dreamed of.
At 19, I had a reduction and my surgeon advised me there would be a 50-70% chance I could breastfeed. When I started to see some colostrum emerging (I never leaked, and had to squeeze my breasts to see any) at 26 weeks pregnant I got giddy at the idea I could actually do it! I went in with a plan, writing in my birth preferences that I wanted to breastfeed our new baby as soon as possible after delivery, ensure that he was not offered formula, and that there was a pump in my room.
Come the day that my son was born, and everything was working against us. He was born via emergency c-section at almost 42 weeks just over 6 lbs - intrauterine growth restriction that was undiagnosed. I couldn't feed him right away, because they had topped up my epidural so much that I could barely speak or keep my eyes open. A few hours after his birth, I was somewhat functional, but the doctors advised me our little one had low blood sugars and needed to eat immediately. He was unable to latch properly due to flat/inverted nipples and he was given a small amount of formula by syringe in hopes we could nurse the next feed. I was brought a hospital pump to try, but wasn't given any assistance with my baby so I didn't have time to pump between his feedings, his glucose checks, visits from doctors/nurses/laboratory (almost hourly) and taking care of my own wounds.
Within a few hours, the nurses advised me he was jaundiced and would need light therapy. He would, preferably, need to be fed while lying under the lights but, I refused and insisted I take him out at feedings to try and have him latch. He couldn't effectively latch and, even though I requested to see an LC as soon as possible, there wasn't anyone available. I was told to try and pump (they provided me a double pump with only 1 pump kit!) in between doing all of the "chores" on their checklist for me - which included complete care of my baby, checking my incision, getting in/out bed to go to the bathroom, charting my son's temperature and calling for glucose checks, filling out paperwork, etc. not once did anyone offer to change a diaper or give him a feed so I could pump.
By the second day the nurse suggested a nipple shield, but the hospital didn't provide them, so I had to wait for a family member to bring me one. In the meantime, the single pump kit was thrown out by custodial staff and not replaced.
By the time I was discharged, 4days later, I had only been able to pump a few times. Our son had successfully latched on a few times with the shield, but screamed 20 minutes after each feed for more milk. A feeding session on the breast was lasting more than an hour at times, and I was told he had to be doing his light therapy if we wanted to go home.
Once we got home, I was told to attempt a strict regimen to up my milk supply - feed/burp the baby on the breast (up to 20 minutes per side), feed the baby formula - making note of how much he ate, then pump each side for 15 minutes, then go to the bathroom/apply new dressings to my incision, make a snack, and try to sleep before he woke for more food. I was able to pump a maximum of 5mL (not ounces) at a time and frequently less, even after my milk "came in". By his 7th day, he would scream himself into a tizzy from hunger so strong that he was unable to latch, even with a shield. Add to that undiagnosed issues with my c-section that required ER visits, nobody at home to help feed him while I attempted pumping (he would scream if I put him down, so I had to try holding him while holding the pump), a one month wait to see an LC, undiagnosed PCOS with high testosterone, and dehydration/not eating enough.
By month 2, he developed Colic and refused to eat at the breast because he had to wait for me to put the nipple shield on. Yes, I did have some drips of milk when he cried, but I could never pump more than 10mL (less than 1/2oz) at a time, sometimes it was 20mL in one day - and I took fenugreek and blessed thistle! Now at almost 4 months, he is exclusively formula fed. I wish I had been able to breast feed - he had two real "meals" at the breast.
Looking back, if I had received more help from the beginning, the outcome would have probably been more favorable, but it wasn't. All I can do is hope our next baby has the opportunity to have something our first couldn't have.
OMG. I am in TEARS! This is the FIRST I've EVER heard about the connections to low milk supply!
My daughter will be 10 this year. Her first week of life was hellish on us (she was baby 1) . I exclusively was breast feeding. This child was clingy, fussy, cried, wouldn't sleep on her own...it was horrible for us. At her 1 week checkup, we discovered she lost more than 10% of her birth weight. The lights started to light up a little...obviously I wasn't producing enough.
I was given a prescription to help produce more, set up with an SNS setup (ugh!), and purchased the best pump out there at advice from the lactation consultant. Pumping produced DRIPS. There was nothing there even to save! It was a heartbreaking experience for me and after a few weeks of doing the SNS, I gave up. Once I set the child up on formula, she was MUCH happier as were my husband and I.
But up until this VERY HOUR, I had NO idea PCOS could contribute. Up until THIS VERY HOUR, I had NO idea of ANY potential causes other than "some women don't produce enough".
All of the struggle back then could have been prevented had I KNOWN! My little girl was HUNGRY and we had no idea she wasn't getting enough. I am heartbroken and ANGRY that nobody told us...
For the most part, my daughter is healthy, thankfully, but she struggles with separation issues (never wants to sleep in her own bed, etc) and sensory issues. I've been living with this horrible guilt wondering if that first week of life of being HUNGRY contributed to some of her neediness even 10 years later. FOR WHAT?! To discover that it could have been prevented had I been forewarned?!?!
Yes! I.AM.BITTER.
I think the international comparisons are a little misleading. You're looking at rates of some breastfeeding, but that doesn't say anything about supply. The rate of EXCLUSIVE breastfeeding at 6 months is at best 10% in Norway. At just 4 months, fewer than half are exclusively breastfeeding. http://www.health.gov.au/internet/publications/publishing.nsf/Content/int-comp-whocode-bf-init~int-comp-whocode-bf-init-ico~int-comp-whocode-bf-init-ico-norway Sweden is similar.
Are we so sure that with all the support and education in the world, a lot of Scandinavian women aren't also struggling with supply issues?
On the flip side, are we so sure that there aren't a lot of Bangladeshi babies who are surviving but still getting suboptimal nutrition from their mothers' milk? According to UNICEF, 64% are EBF until 6 months, but that means 36% are not. http://www.unicef.org/infobycountry/bangladesh_bangladesh_statistics.html#100 If more than a third of women are supplementing in a country where alternatives are extremely limited and BF is readily accepted, it's hard to imagine that only rich, spoiled westerners are imagining supply problems.
I think the international comparisons are a little misleading. You're looking at rates of some breastfeeding, but that doesn't say anything about supply. The rate of EXCLUSIVE breastfeeding at 6 months is at best 10% in Norway. At just 4 months, fewer than half are exclusively breastfeeding. http://www.health.gov.au/internet/publications/publishing.nsf/Content/int-comp-whocode-bf-init~int-comp-whocode-bf-init-ico~int-comp-whocode-bf-init-ico-norway Sweden is similar.
Are we so sure that with all the support and education in the world, a lot of Scandinavian women aren't also struggling with supply issues?
On the flip side, are we so sure that there aren't a lot of Bangladeshi babies who are surviving but still getting suboptimal nutrition from their mothers' milk? According to UNICEF, 64% are EBF until 6 months, but that means 36% are not. http://www.unicef.org/infobycountry/bangladesh_bangladesh_statistics.html#100 If more than a third of women are supplementing in a country where alternatives are extremely limited and BF is readily accepted, it's hard to imagine that only rich, spoiled westerners are imagining supply problems.
As a woman with low supply who has tried to breastfeed through 4 children, I agree most with what Kate said.
Often women with low supply are let down by the breastfeeding community because they rely on the idea that if your child does not have enough milk it is because you are not working hard enough.
They're not there when:
*your baby is diagnosed failure to thrive
*you're threatened with formula feeding or the child will be removed from your care
*the severe jaundice
*the stinky teas and horsepills
*your baby starts crying when you unbutton your shirt to feed them
*your child eventually refuses the breast
*you nurse, then formula feed, then pump, then feed what you pumped, and then start all over again without a break
*the lactation consultants who offer helpful hints like "you must be doing it wrong" or "stop being so lazy!" "just work harder...any woman can do this."
After a few months of this, the lack of sleep, the crying, the "helpful" people who tell you to just work a little harder, it would be a miracle if any woman in this position kept breastfeeding. I still have PTSD thinking about those years.
It wasn't until my third child that I regained some peace about the whole thing. I joined an online group called MOBI (Mothers and Others with Breastfeeding Issues). I don't have a diagnosis. I was obese as a teen and lost the weight later. I'm borderline hypothyroid. One side of the family has Type2 diabetes issues and I'm sensitive to sugar. Whatever happens to be my particular problem, I've accepted it. That doesn't mean doctors, nurses, and lactation consultants have, but I have.
I tandem breastfed and formula fed from day 1 with my third child, always breast first. He nursed 11 months. The numbers were similar with my fourth. I'm very proud of that.
Hugs Tamara I am right there with you. I met with several lactation consultants all of whom told me I would never exclusively breastfeed my twins and not to worry about it because supplementing was ok. I refused to believe them though because the misinformation on the internet is that the reason you aren't producing is because you are lazy or you don't love your kids enough. I spent their first 3 months weeping as they got skinnier and skinnier. When I finally gave in and added formula they thrived. I still get very depressed about it even though I know there was nothing I could have done it still makes me feel like a failure as a mother. Thr truth is Bangladesh may have higher breastfeeding rate but their infant mortality rate is also almost 6 times higher.
Another factor, not listed in this article or their long list of other possible causes, can be stress and Post-Partum Depression. That was, I think, the case with me.
Do you have interest in a loan if yes apply via: raybenchris_loan@outlook.com
Loan application form fill and get back on time
Name:
County:
City:
Amount;
Duration:
Sex:
Phone number:'
Purpose of loan:
Have you apply before:
Regard
Mr williams
For me at first it was hard but then I discovered A lactation tea by Secrets Of Tea that helped me increase my milk supply and it tastes amazing, I also ate a lot of oatmeal because they say it helps
I was coping with low breast milk and it was really a challenging to satisfy my child who was not taking any supplement. I tried different cookies, mothers milk and other things including massage, but the final thing that boosted my supply was healthy nursing tea by secrets of tea.
I just wanted to say thank you for this post. I too felt an absolute failure when I couldn't make enough milk and had no idea it was to do with my PCOS till ages later. My lo dropped over a lb in a few days, my breasts never felt 'full', never pumped more than 5ml etc - but all you hear is "only 5% of women are unable to produce enough milk..." as if I couldn't possibly be one of them, and I just wasn't trying hard enough. I wish I'd known sooner so I could forgive myself sooner.
I was coping with low milk supply and struggling hard to get it boosted. I ate cookies, drank mother's milk, and many more home remedies but the result was the same. My LC suggested me a herbal tea healthy nursing tea. I started drinking this tea and it gave me much better results.
Practical blog post - Speaking of which , if your company has been searching for a a form , my business partner filled out a template form here
http://goo.gl/0uZ3cZThank you so much for this wonderful article! I have a 7 week old, my fourth child, and have always struggled with breastfeeding and then given up due to low milk supply. I have an under active thyroid as well as pre-diabetes, and had no idea that these were related to my milk troubles. My question now is that is there hope that my milk will increase? My son is 7 weeks and is pretty much formula fed as I'm producing very little milk. If I pumped more often (as I was told to by my LC, but haven't been able to) would I see an increase or is it too late?
I waant to answer Sadis email. I would say sure its not too late you should try pumping more anyway! Plus make sure you breastfeed her at least eight times a day (ten maybe until shes two months of age if needed) I started out giving lots of formula and eventually started being able to incorporate more pumping until I didnt have to give any formula. In my opinion its natural to find it hard to pump until you get used to it and gradually find ways to squeeze it in. You also get stronger as time goes by both emotionally and physically and that allows you to find the energy to do more things... That said five am is when prolactin peaks so make sure you do your early morning pumpings for sure! You can pump between 15 and 30 mins so maybe even pump longer for a pumping where youre getting more milk! I have a four and a half month year old and have no idea whether I have low supply but always wonder if I do or whether baby still has suction problems or just nipple confusion.
At 7 weeks I was pumping three times and now I pump six to eight times. When baby was one week old she had lost ten percent of her weight so we had to give her some expressed milk and formula. And then she steadily gained weight until recently when she got diarrhea.
I also had the experience where LCs never even rationally consider the possibility of low supply, only the OB does but Im not clear as to how anyone could diagnose it for sure. They also dont realize how very complicated it is to supplement and breastfeed and pump at the same time!! Maybe because they havent ever done it...Its insane but I keep looking for solutions. Such as trying to reduce the supplement gradually by one oz a day like kellymom.com advises.
Both my boys had tongue and lip ties that affected my supply. Little did I know with my first till he was almost 2 so with the second I had the ties released and he's gaining beautifully. Apparently it's very common but most pediatricians and lactation consultants aren't specialists in this area. I had to take my little one to a pediatric dentist to have it evaluated and he went from gaining 1/2oz to 1oz a day.
Drinking Sage Leaf Tea is also be the good home remedies to decrease breast milk.
Well...Also, in India, babies of mothers with low supply are more likely to have died from malnutrition. Here, we are more likely to catch the problem.